August 18, 2022— A pair of recent studies add to the growing body of research concluding that hospitals participating in the 340B drug pricing program are providing the lion’s share of care for patients who are most in need. These include people who cannot afford the services they need and people who historically have been underserved by the broader health care system. The researchers say the data provide important evidence that 340B is a critical part of our health care safety net and national efforts to pursue greater equity in health care.
Rising to the COVID-19 Challenge
Uncompensated and unreimbursed care is one measure of hospitals’ service to patients living with low incomes. It includes care provided to uninsured and underinsured patients who cannot afford their hospital bills. It also includes care for patients covered by Medicaid and other programs that do not pay hospitals the full costs of delivering that care.
A July 20 report by Dobson DaVanzo & Associates analyzed Medicare cost report data to determine how much uncompensated and unreimbursed care 340B disproportionate share (DSH) hospitals provided their patients in fiscal year 2020. In early 2020, the nation began to confront the COVID-19 public health emergency. The researchers sought to see what effect the onset of the pandemic had on those hospitals’ ability to serve their patients.
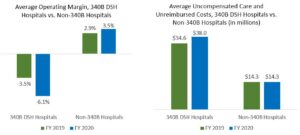
The COVID pandemic hit the finances of 340B hospitals particularly hard, the research found. Hospitals saw spikes in the costs of caring for COVID and non-COVID patients combined with decreased payments from cancelations of elective procedures and other nonacute care. Prior to the pandemic in FY 2019, these safety-net hospitals already had an average annual operating margin that was negative, meaning the typical hospital brought in less in operating revenues than it spent in operating costs. In FY 2020, that average figure plummeted. Although hospitals received assistance from the government through COVID relief funding, the support provided to 340B hospitals was not enough that it would have put their average operating margin into the black.
Despite this financial battering, the researchers found 340B hospitals increased the amount and share of uncompensated and unreimbursed care they provided during the fiscal year. That figure rose by billions of dollars as the pandemic hit, to the point where 340B hospitals provided more than $41 billion, or two-thirds of all such care in the U.S. For non-340B hospitals, operating margins increased in FY 2020 while uncompensated and unreimbursed care stayed flat.
When Congress established 340B nearly 30 years ago, it stated that drug discounts would enable safety-net hospitals to stretch their resources further to provide more care and serve more patients. The pattern of 340B hospitals providing more care to patients in need while under great financial duress “provides important evidence that 340B DSH hospitals are continuing to fulfill the program’s purpose as set out by Congress in 1992,” the researchers conclude.
Serving the Underserved
The pursuit of health equity involves acknowledging that the U.S. health care system has not provided equitable care to all patients regardless of their background or circumstances. People living with low incomes, people with disabilities, and people of color have encountered more challenges to health care access and an elevated disease burden.
A July 28 report by L&M Policy Research analyzed 2019 federal data to determine the extent to which patients in these demographic groups received their care from 340B hospitals, non-340B hospitals, and physician offices. The study’s purpose was to compare how different types of providers were serving the historically underserved.
The researchers found that the patients receiving care at 340B hospitals are significantly more likely to be a member of one of the historically underserved groups than those who receive care at non-340B hospitals or doctors’ offices. The categories include:
- Patients who are eligible for both Medicare and Medicaid, typically because they are living with low incomes or significant disabilities
- Medicare patients who are disabled
- Medicare patients under age 65 who are eligible because of a disability or severe disease state
- Patients who identify as Black
“These findings reinforce previous analyses documenting that 340B is working as Congress intended, supporting hospitals that disproportionately serve people experiencing low incomes and other underserved populations,” the report concludes. “As policymakers consider changes to the 340B program, they should consider the impact changes would have on patients served by 340B safety-net hospitals.”
Maintaining a Strong Safety Net
Both the work to help bring about the end of the COVID-19 pandemic and the pursuit of greater health equity continue today, and all health providers are part of these campaigns. The recent research demonstrates that the safety-net hospitals participating in 340B have outsized roles to play in the efforts.
“Patients who are most in need are much more likely to rely on 340B hospitals for their care, and those hospitals use their 340B savings to provide additional services and reduce inequities in care,” said Maureen Testoni, president and CEO of 340B Health. “By doing so, 340B serves as a cornerstone in the continuing effort to build more access and equity into the health care system.”