October 20, 2022— A pair of new research reports adds to the growing body of evidence of the critical role 340B hospitals play in caring for patients living with low incomes. The research also demonstrates the crucial part these hospitals played in the initial stages of the COVID-19 pandemic.
To qualify for 340B drug discounts, most hospitals must document that they serve a “disproportionate share” of patients with low incomes who are enrolled in Medicaid or Medicare. These “DSH” hospitals must prove they meet that requirement each year to renew their 340B status. Earlier research looking at fiscal year 2015 data showed 340B DSH hospitals provided about 60% of all uncompensated and unreimbursed care. This care is an important measure of hospital care for low-income patients because it includes:
- Financial assistance to patients whom the hospital determined could not pay for their care
- Underpayments by state Medicaid programs
- Services for which hospitals anticipated but did not receive payment due to a patient’s inability to pay, known as “bad debt”
The research found DSH hospitals also are much more likely to provide services that private and public insurance do not cover, including transportation and translation services as well as medical management programs that help patients understand and keep to their treatment plans.
Those same researchers went back and looked at fiscal year 2020 data from the Centers for Medicare & Medicaid Services (CMS) to see if those numbers had changed. This fiscal year included the initial months of the COVID-19 pandemic in the U.S. During the early months of the pandemic, many hospitals postponed or canceled elective surgeries and the numbers of patients they served dropped dramatically. At the same time, the patients they were serving tended to be older, sicker, and more costly to treat.
The new report by Dobson DaVanzo found 340B DSH hospitals’ operating margins had fallen sharply from an average of -3.5% in 2019 (the year before the pandemic) to -6.1% in 2020. While some of those losses were offset by emergency federal funding as part of the national response to the pandemic, 340B DSH hospitals, on average, remained in the red. By contrast, non-340B hospitals saw their already positive margins grow from an average of +2.9% to +3.5% and their provision of uncompensated care remained flat.
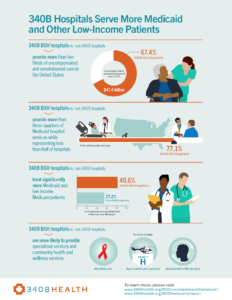
The researchers also explored how the pandemic and the sagging economy affected 340B DSH hospitals’ provision of uncompensated and unreimbursed care. What they found reinforces the crucial role these providers are playing. In FY 2019, these hospitals provided $34.6 billion in such care. In FY 2020, that amount rose to $38 billion, which represented 67% of all uncompensated and unreimbursed care in the U.S.
Caring for Patients with Low Incomes
Congress created 340B in 1992 to help shore up the health care safety net so patients – especially those with low incomes – can access needed care. Dobson DaVanzo looked at FY 2020 data to see how 340B DSH hospitals fulfill that role. They found the hospitals provided 77% of all hospital care – inpatient and outpatient – for people with Medicaid.
The fact that Medicaid patients make up such a sizable proportion of people receiving care at 340B DSH hospitals is further evidence of the role 340B savings play in supporting the safety net. According to the American Hospital Association, hospitals received payment of only 88 cents for every dollar spent by hospitals caring for Medicaid patients in 2020. A non-340B hospital can recoup those losses by caring for a larger proportion of privately insured patients, because private insurance tends to pay closer to the actual cost of delivering care.
One final piece of evidence comes from the report’s accounting for the types of services that 340B DSH hospitals offer compared with non-340B hospitals. Here, Dobson Davanzo found 340B facilities are much more likely to offer such vital services as burn, trauma, and neonatal intensive care. 340B DSH hospitals also are more likely to offer services important to underserved populations such as HIV/AIDS and behavioral health services.
A Large and Growing Body of Research
The growing compendium of published research documenting the positive impact of 340B on the safety net and the low-income patients it serves is a hallmark of the 30-year history of the program. Three decades after a bipartisan majority of Congress voted to approve 340B and a Republican president signed it into law, the evidence is clear that it continues to fulfill the vital role it was designed to play.